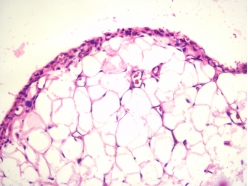
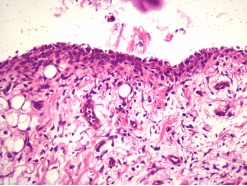
Model Introduction
Osteoarthritis (OA) is a class of chronic degenerative diseases characterized by articular cartilage degeneration, subchondral bone changes, and synovial inflammation. Recent studies suggest that OA is not a single disease but exists in different phenotypes, including:
- Traumatic OA
- Metabolic OA
- Aging-related OA
- Genetic OA
- Pain-related OA Different phenotypes exhibit significant differences in pathological mechanisms and treatment responses; therefore, reasonable and stable animal models must be established based on phenotypic characteristics.
Research Applications
OA animal models can be used to:
- Study the pathological mechanisms of different OA phenotypes.
- Evaluate chondroprotective and repair treatments.
- Explore the roles of inflammatory cytokines and metabolic abnormalities.
- Study age-related OA progression.
- Evaluate the efficacy of analgesic and anti-inflammatory drugs. Phenotypic modeling helps improve research precision.
Experimental Design Key Points
I. Traumatic OA Model
(A) Invasive Induction Methods
- ACLT (Anterior Cruciate Ligament Transection)
- Simple operation, minimal structural damage.
- Progression is slower than MMT, suitable for pharmacological research.
- Evaluated using Mankin or OOCHAS scores.
- Vibration or weight-bearing training can accelerate model progression.
- MMT (Medial Meniscal Transection)
- Faster progression than ACLT.
- Commonly used for short-term studies.
- Can simulate early OA within 4 weeks.
- Modified Hulth Method
- Retains part of the ligaments.
- High success rate.
- Forced exercise can shorten the cycle.
- Closed Joint Scoring/Groove Method
- Minimal trauma.
- Suitable for early OA research.
(B) Non-invasive Induction Methods
- Intra-articular Tibial Plateau Fracture Method
- Controlled impact force.
- Applicable for acute injury research.
- Cyclic Joint Compression Method
- Simulates chronic overuse.
- Different loads produce different levels of severity.
- Tibial Compression Overload Method
- Single high-energy impact.
- Suitable for early OA research.
II. Metabolic OA Model
- High-Fat Diet Model
- Does not destroy joint stability.
- Close to the mechanism of obesity-related OA.
- Usually requires approximately 20 weeks for modeling.
- Ovariectomy Model
- Simulates estrogen imbalance.
- Can be combined with exercise to accelerate progression.
- CTX-I and CTX-II are associated with degeneration.
III. Aging-Related OA Model
- Natural Aging Model
- Hartley guinea pigs are commonly used.
- Pathologically similar to humans.
- Anti-aging Gene Knockout Model
- e.g., SIRT1 knockout.
- Can be combined with ACLT+MMT to establish advanced-age models.
IV. Genetic OA Model
Relevant genes include:
- Col11a1, Col2a1, Del1
- Type II and Type IX collagen
- Copper transport genes
- MMP-13, BMP-1a receptor, ADAM-15, MMP-14
- IL-6, Mig-6, A-1 integrin
- Fibromodulin, Biglycan, etc. Suitable for genetic mechanism research and efficacy evaluation.
V. Pain-Related OA Model
(A) Intra-articular Injection Method
- Monosodium Iodoacetate (MIA)
- Inhibits the Krebs cycle.
- Induces chondrocyte apoptosis.
- Pain severity correlates with dose and time.
- Classic pain model.
- Papain
- Induces cartilage destruction.
- Early OA forms in 4–6 weeks.
- Collagenase
- Degrades cartilage matrix.
- Pathological changes visible in 3 days.
(B) Cold Stimulation Method
- 4°C fixation.
- Cartilage damage appears after 6 weeks.
- Elevated levels of IL-1β, TNF-α, etc.
(C) Blood Circulation Blockage Method
- Vein ligation.
- Early to mid-stage OA forms in 8 weeks.
Key Detection Indicators
- Cartilage histological scores (Mankin, OOCHAS).
- Subchondral bone changes.
- Inflammatory cytokines (IL-1β, TNF-α, etc.).
- CTX-I, CTX-II.
- Imaging evaluation.
- Pain behavioral assessment.